Removal of fibroids by laparoscopy (Laparoscopic Myomectomy) is perhaps the most tedious of all laparoscopic surgeries. There are many steps namely:
- Devascularize the uterus
- Removal of the fibroids
- Repair the defect
- Removal of the fibroid/s by morcellation
My biggest fear when performing myomectomy by laparoscopy is missing fibroids. There are several strategies for not missing a fibroid when performing this surgery. They are:
- Transvaginal ultrasound during the surgery
- Transvaginal injection of methylene blue dye on the capsule of the fibroid
- Minilaparotomy
- Intraoperative ultrasound
This can be done easily. Once all the visible fibroids are removed by laparoscopy, a transvaginal ultrasound (TVS) can be done to look at the uterus to see if there are any fibroids that are still remaining in the uterus. One trick is to place some fluid in the Pouch of Douglas and place the patient in the reverse Trendelenburg position when performing the transvaginal ultrasound. The advantage of this method is that it is easy to find an ultrasound with a transvaginal probe. However, there are several disadvantages. Firstly, in virgo intacta patients TVS cannot be done. This can be overcome by performing a transrectal ultrasound. The biggest disadvantage I face with this method is that, it is difficult to determine the place on the uterus to make the incision having located the fibroid by transvaginal ultrasound. The orientation can be difficult.
Transvaginal injection of methylene blue dye into the capsule of the fibroid.
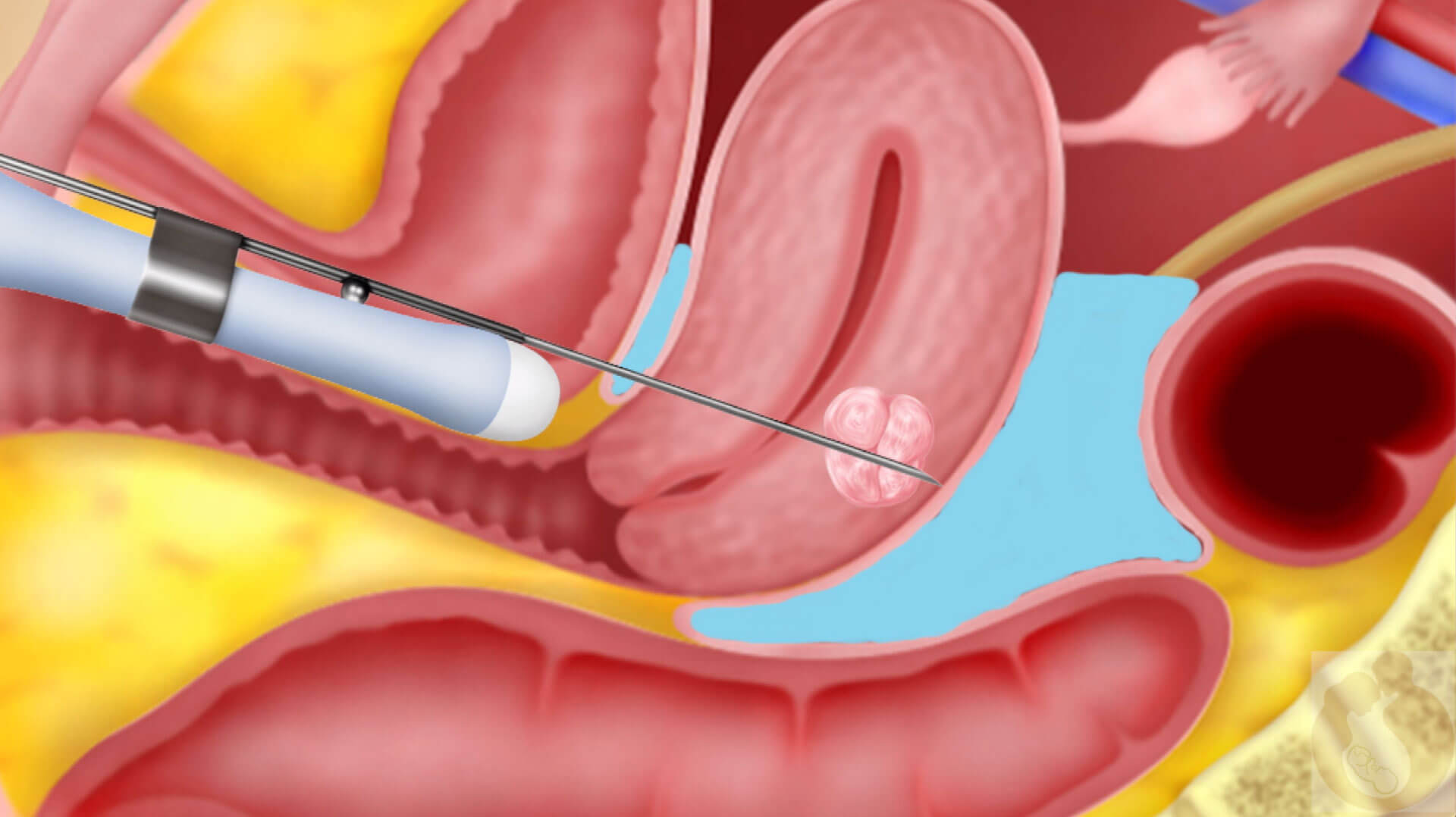
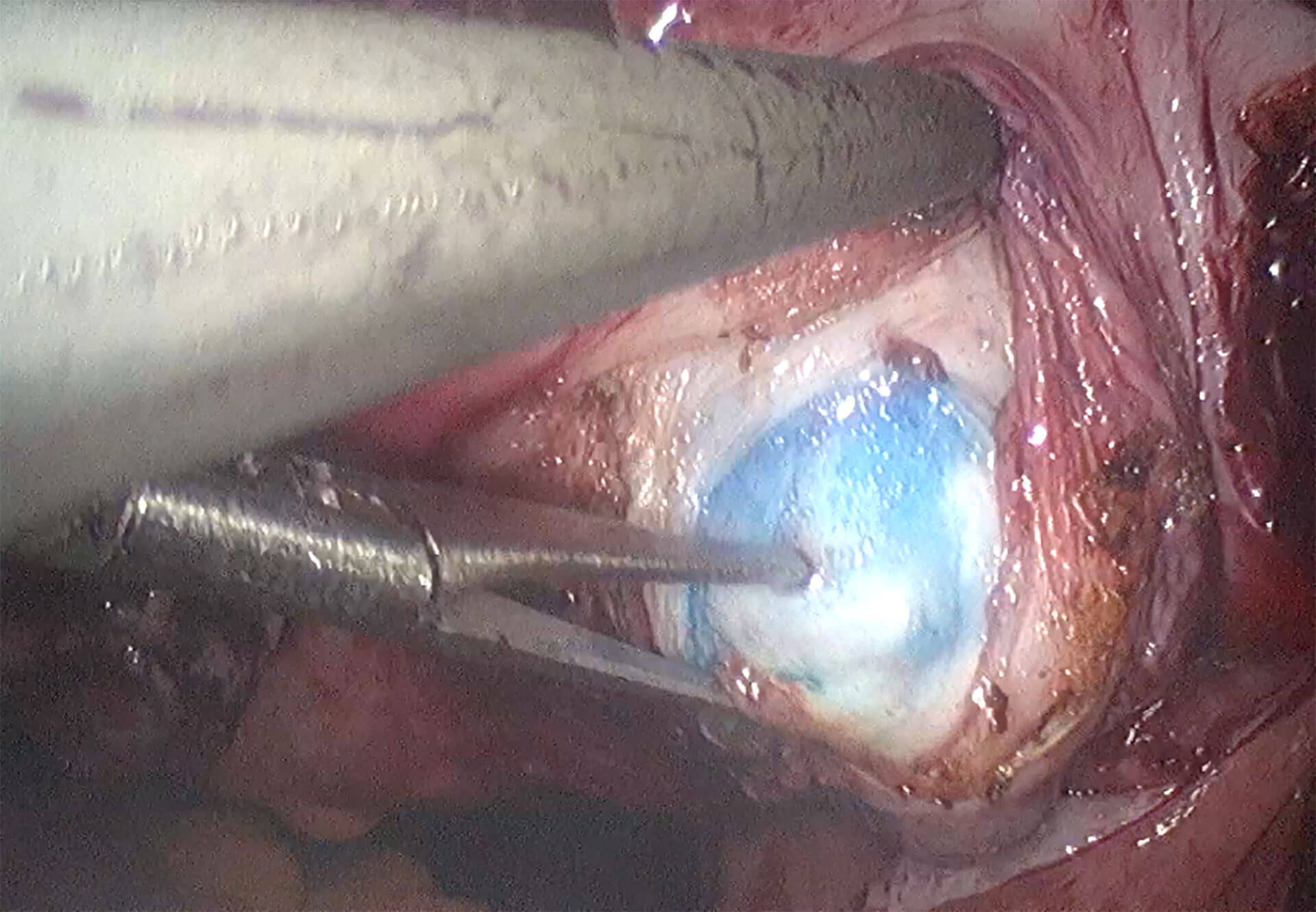
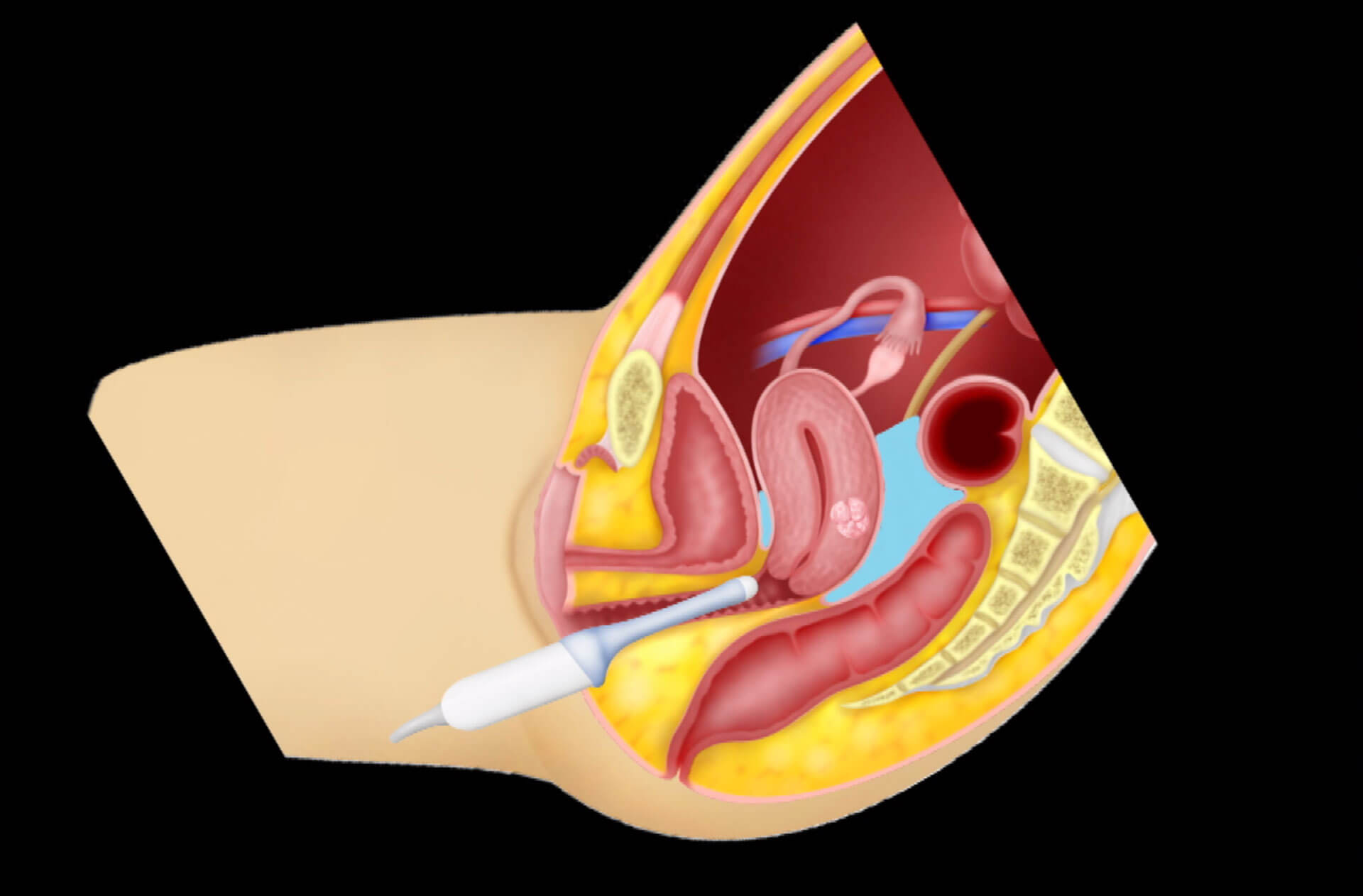
When a fibroid is seen on transvaginal ultrasound and it is difficult to know where to cut on the uterus laparoscopically, one strategy is to place a needle vaginally (similar to oocyte retrieval ) and inject methylene blue into the capsule of the fibroid. When this bluish tinge is seen laparoscopically, we will be able to know exactly where to make an incision on the uterus to locate the fibroid.
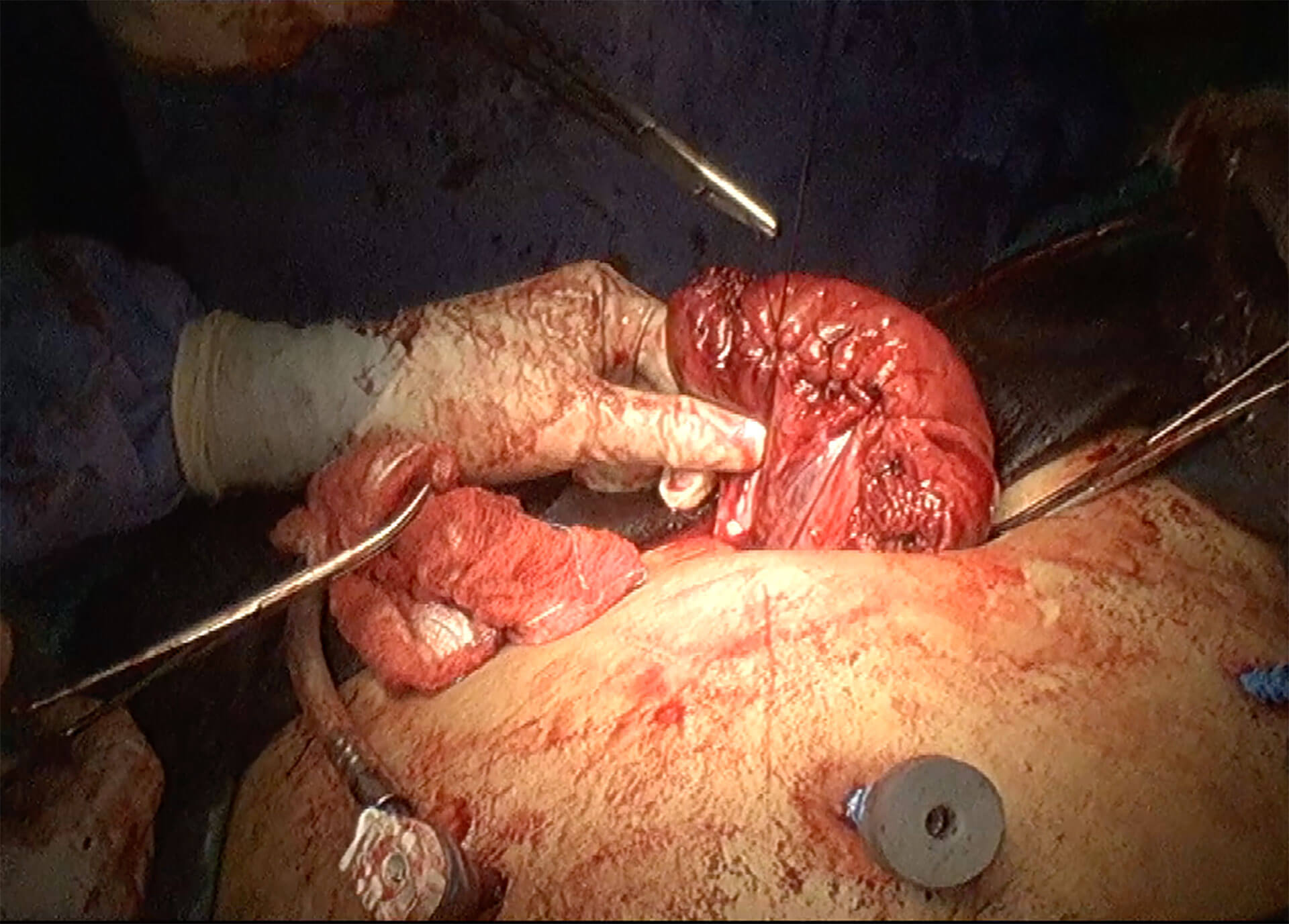
In patients with multiple fibroids some big and some small, instead of performing a large laparotomy incision, I perform a laparoscopy to remove all the big fibroids first and then perform a minilaparotomy. There are 2 advantages of the minilaparotomy. Firstly all the big fibroids that had been removed laparoscopically can be removed through this minilaparotomy incision. Secondly, I can pull out the small uterus through the minilaparotomy incision, feel the uterus with my hands and remove all the remaining small fibroids. In this way, I am sure of having removed all the fibroids. I will then repair the uterus and then replace the repaired uterus into the abdomen. A laparoscopy is then performed after that. It will be easier to place antiadhesions on the repaired uterus. In this strategy, I have converted a large laparotomy into a suprapubic transverse minilaparotomy. As the uterus is pulled out of the abdomen, there is no manipulation of the intestines by the hands of the surgeon. This will lead to less intra abdominal adhesions.
BK Medical® makes an ultrasound machine with intraoperative ultrasound probes. The ultrasound probes can be inserted into the abdomen through a 10mm trocar. After laparoscopic removal of all the fibroids, the probe can be placed on the uterus. Intraoperative ultrasound can be done to locate any fibroids left in the uterus. If a fibroid is seen by ultrasound, an incision can be made on the uterus exactly where the intraabdominal probe was placed and the fibroid can be removed easily. This is perhaps the best way of locating a fibroid that could not be visualised during laparoscopy. The only problem is that BK Medical® is the only company that makes this intraoperative ultrasound probe and the machine is expensive.
Please watch the video at:
https://www.youtube.com/watch?v=1KBuEdJ0G0g&t=6s
https://vimeo.com/manage/400540617/general
Dr. Selva
Sevellaraja Supermainam
23/3/2020






