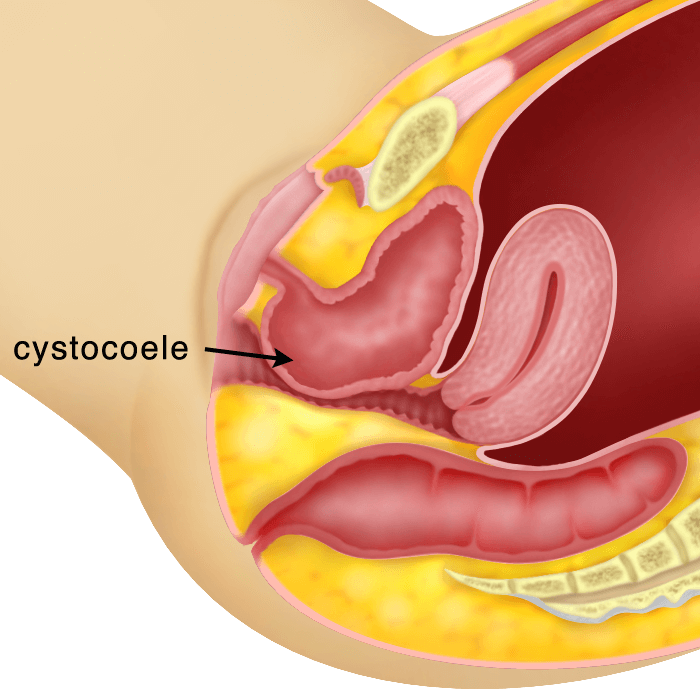
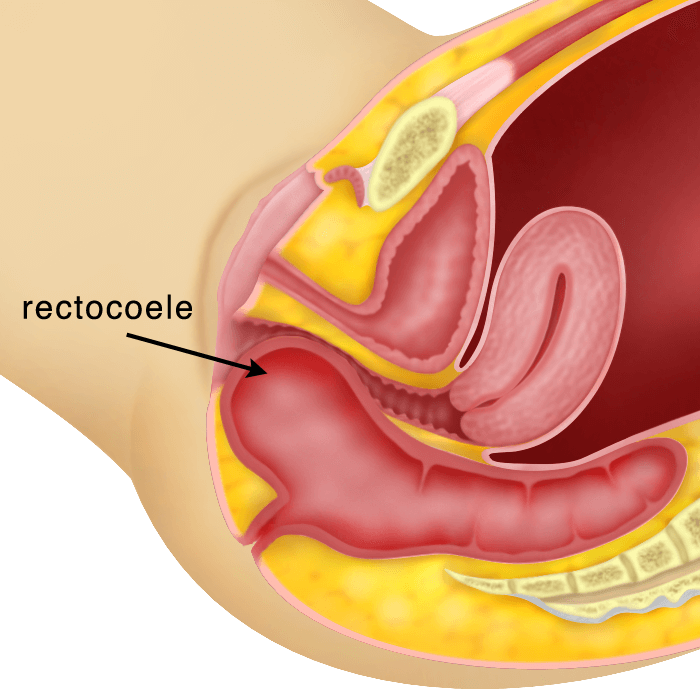
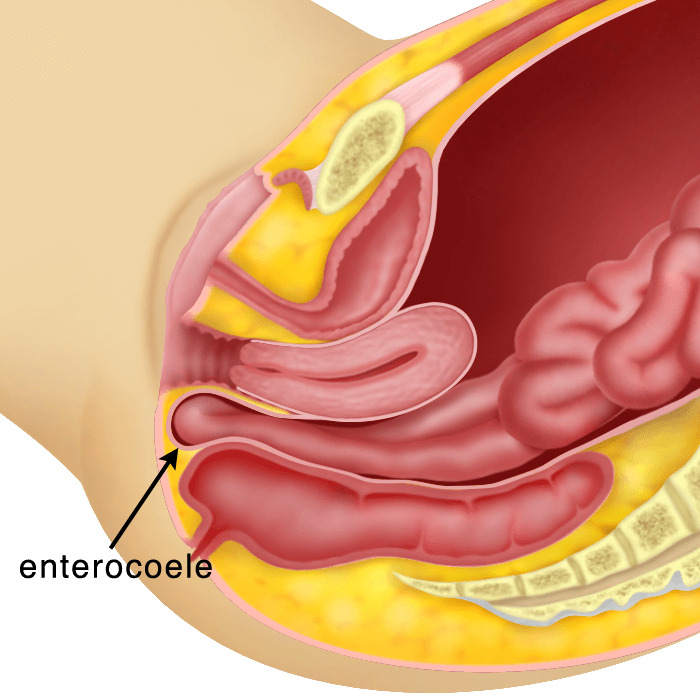
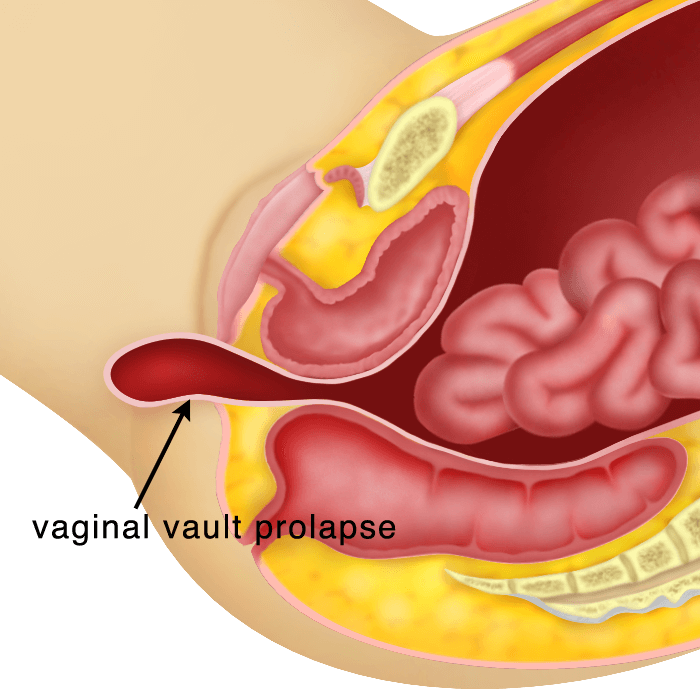
Utero-vaginal Prolapse is a condition whereby the uterus protrudes or descends down the vagina and sometimes out of the vaginal opening (introitus). This condition may occur together with the descent of the bladder (cystocoele), the rectum (rectocoele), the intestines through the back part of the uterus (enterocoele) or the descent of the urethra (urethrocoele). Sometimes the vagina can descend after a hysterectomy. This is called a vaginal vault prolapse.
Degrees of Utero-vaginal Prolapse
The extent of descent of the uterus determines the severity of the prolapse. This is generally divided into 3 degrees:
First degree Utero-vaginal Prolapse
The uterus sags down up to the introitus but remains within the vagina.
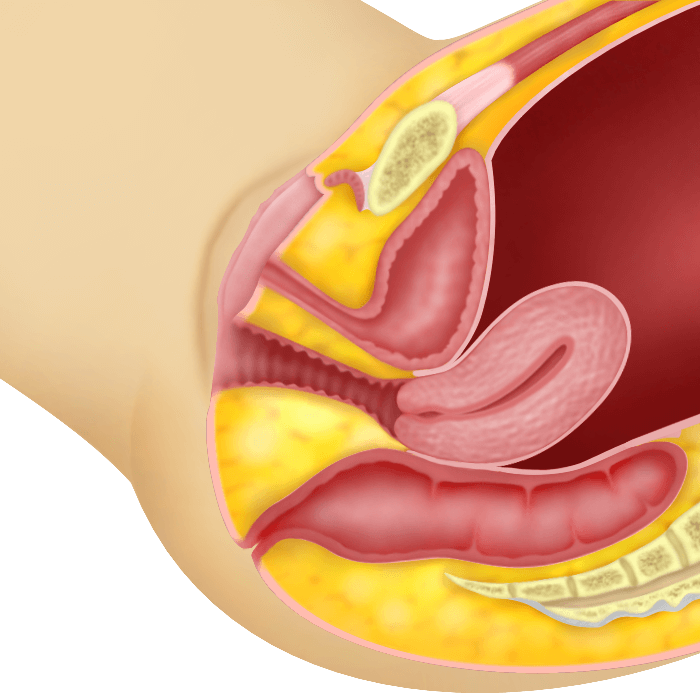
Second degree Utero-vaginal Prolapse
Here, the cervix protrudes out of the vaginal opening but the body of the uterus still remains in the vagina
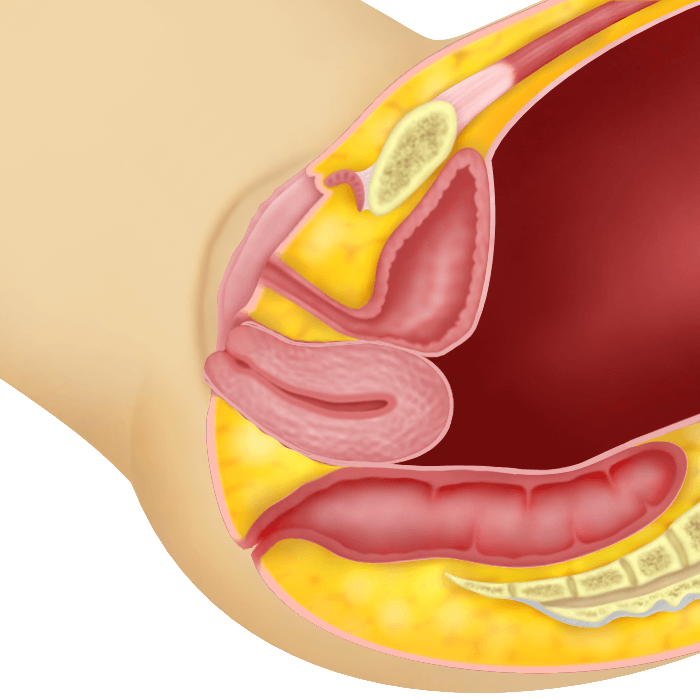
Third degree Utero-vaginal Prolapse
The whole uterus has protruded out of the vaginal opening
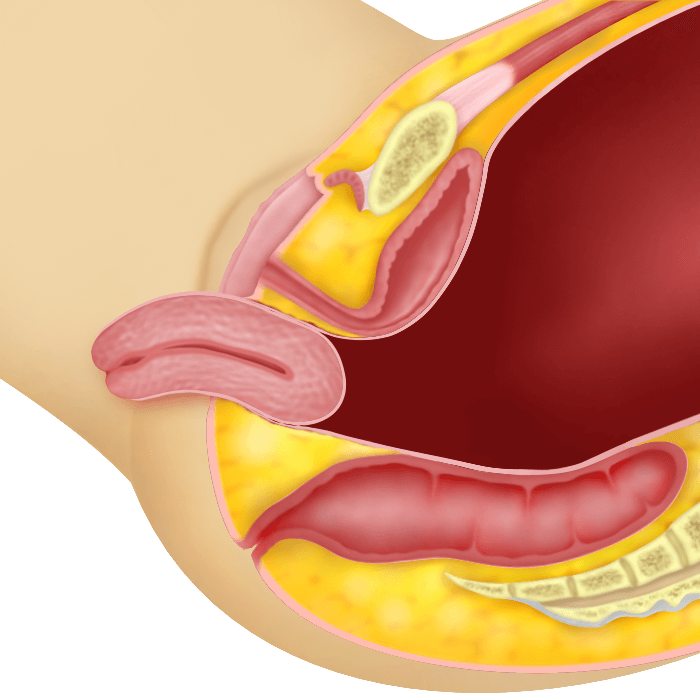
Causes
Utero-vaginal Prolapse occurs when there is a weakening of the tissues that support the uterus. There are several reasons why utero-vaginal prolapse occurs:
1) Difficult childbirth. Women who have delivered large babies or have had difficult labour, have a higher risk of developing utero-vaginal prolapse. A difficult childbirth can cause muscle weakness and stretching of the tissues supporting the uterus. This could lead to a prolapse in the future.
2) Menopause: After menopause, a lack of the hormone oestrogen causes the loss of muscle tone associated with ageing. This may lead to prolapse.
3) Diseases that increase the intra-abdominal pressure such as chronic cough, severe constipation and pelvic tumours can occasionally lead to or aggravate a prolapse of the uterus.
Risk factors for pelvic organ prolapse include the following:
1) Increasing age
2) Increasing body mass index (obesity)
3) Increasing gravidity (g).
4) Increasing parity (g).
5) Number of vaginal deliveries
6) Macrosomic (big baby) delivery
7) Chronic obstructive pulmonary disease (g).
8) Constipation
9) Strenuous activity, weight bearing, or strenuous labour
Symptoms
Many women may have mild utero-vaginal prolapse and not have any symptoms at all. Some, however, will feel the symptoms below:
1) Feeling of a mass coming down the vagina
2) Dragging sensation or discomfort in the lower abdomen or pelvis
3) Back ache
4) Difficulty or inability to completely move the bowel (constipation)
5) Difficulty or incomplete emptying of the bladder
6) Leakage of urine (incontinence) during coughing, straining or sneezing.
7) Vaginal discharge or bleeding
8) Feeling of loosening of the vaginal tone during sexual intercourse
Prevention
It may be difficult to prevent the occurrence of an utero- vaginal prolapse. However, the following strategies may reduce the incidence of a prolapse:
1) Pelvic floor exercise: Performing pelvic floor exercise on a regular basis will help strengthen the pelvic floor muscles. This is especially important after childbirth.
2) During labour: Avoid bearing down (pushing) before the cervix is fully dilated
3) Treat and prevent constipation. Drink plenty of water and eat high fibre food
4) Control chronic cough
5) Avoid lifting heavy objects. Use your legs instead of your waist and back when lifting.
6) Maintain an ideal body weight
Treatment
There are several treatment options
1) Pelvic floor exercise
In a mild form of utero-vaginal prolapse, pelvic floor exercises may assist in strengthening the pelvic floor muscles. This may not improve the prolapse but may slow down the worsening of prolapse.
2) Pessary
A pessary is a plastic ring that can be placed in the vagina to push the cervix and uterus up. This method is suitable for women who cannot undergo surgery, due to other health problems and those who are not sexually active. The pessary will need to be cleaned and replaced regularly. Most women can lead a healthy life style with the pessary. Oestrogen cream is usually given to keep the vaginal tissue moist and to prevent ulceration of the vagina.

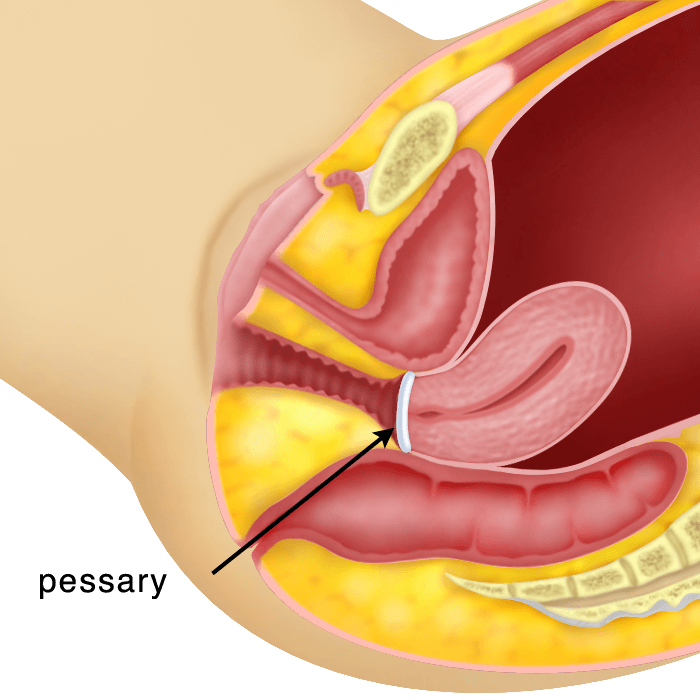
3) Surgery
There are many different surgeries that can be performed for utero-vaginal prolapse. Surgery can either be done via the vaginal route or the abdomen. Surgery via the abdominal route can be performed either by a laparotomy or by laparoscopy.
a) Vaginal Route
There are several surgeries that can be performed via the vaginal route (surgery through the vagina). This includes vaginal hysterectomy and pelvic floor repair, Manchester repair and vaginal mesh placement.
i) Vaginal Hysterectomy and Pelvic Floor Repair
This surgery is performed on women who have completed their families (no desire to have any more children) and are not keen on retaining their uterus. This is the most common surgery performed for utero-vaginal prolapse. Vaginal hysterectomy is usually performed under spinal anaesthesia. The entire surgery is performed via the vaginal route. If there is an associated cystocoele (bladder descent), the bladder
is separated from the vaginal skin and then the tissues are sutured together so as to push the bladder into the abdomen. This surgery is called anterior colporrhaphy. If there is a rectocoele or enterocoele, these can be repaired as well.
The advantage of this surgery is that it is generally an easy operation that can be performed under spinal anaesthesia. The postoperative recovery is quicker as there are no abdominal incisions (no cut in the tummy). The disadvantage of this operation is that the incidence of recurrence of the prolapse
is high especially in women who have poor pelvic tissues for support. Another disadvantage is that the vagina becomes narrow and this may lead to painful sexual intercourse, postoperatively. It is also difficult to remove the ovaries vaginally.
ii) Manchester Repair
This surgery can be performed on patients who have a mild prolapse and wish to retain their uterus. In this surgery, part of the cervix is removed and part of the support of the uterus (namely the cardinal and uterosacral ligaments) are tightened and attached to the cervix to push the uterus into the abdomen.
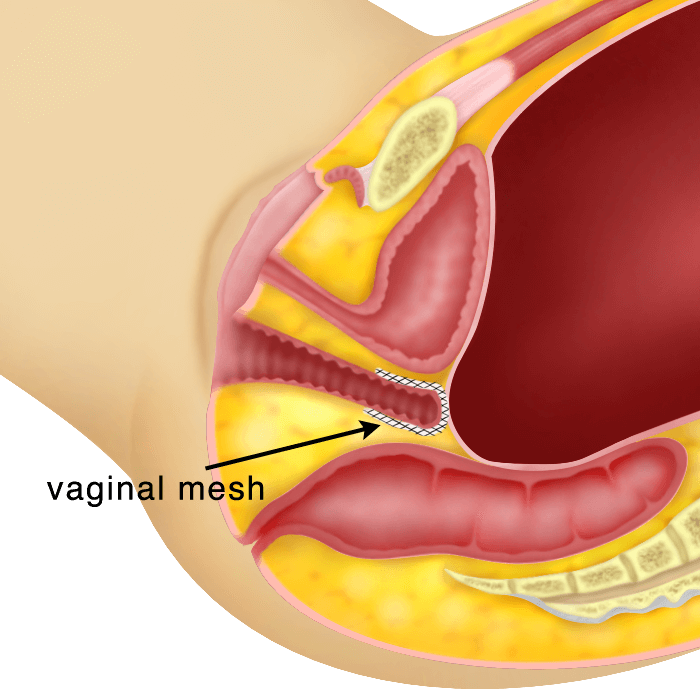
iii) Vaginal Mesh placement
A mesh is a synthetic, permanent material with many holes in
it. The mesh provides additional support by allowing the body’s own tissue to grow into it. In utero-vaginal prolapse, the mesh is usually placed after a vaginal hysterectomy. It is placed under the vaginal skin (above the vagina). To keep the mesh in place, the mesh may have “arms “ that exit through a few small incisions made additionally at the thigh and/or buttocks. Many different types of mesh are available in the market. The advantage of vaginal mesh placement is that it is placed vaginally and so
the operation is relatively simple. The chances of recurrence of prolapse are fewer with meshes as compared to just using sutures to support the vaginal vault. However, there are several possible complications with vaginal mesh placement. This includes mesh exposure, which may lead to vaginal discomfort during sexual intercourse and blood staining or spotting. Some women may suffer buttock and groin pain or chronic vaginal pain. There is also a possibility that the mesh may become infected.
b) Abdominal Route
Surgery via the abdominal route can either be by laparotomy or laparoscopy. Laparoscopy is often advised. The laparoscopic route is the preferred choice. Different types of surgery can be performed. There are 2 ways of reinforcing the tissues that support the uterus. The first is to use mesh and the second is to use sutures. Surgery can be done with or without the removal of the uterus. If a mesh is used, it is usually sutured to the uterus, cervix or vaginal vault and then attached to the sacral promontory (g) (sacrocolpopexy).
If sutures are used, usually non-absorbable sutures are used to:
i) attach the levator ani muscles to the vagina
ii) attach the sacrospinous ligament to the vagina
iii) shorten and attach the uterosacral ligaments together and to the vagina.
The different combinations of surgeries are listed below:
With hysterectomy
i) Subtotal hysterectomy and sacrocolpopexy
ii) Total laparoscopic hysterectomy and sacrocolpopexy
iii) Total laparoscopic hysterectomy and sacrospinous fixation of the vaginal vault
Without hysterectomy
i) Plication of the uterosacral ligaments and round ligaments
ii) Sacrocolpopexy with retention of the uterus
Post hysterectomy; Vaginal vault prolapse
1) Sacrocolpopexy of vaginal vault for vaginal vault prolapse
2) Vaginal vault suspension with sutures
All these surgeries are discussed in detail in chapter 32.
Generally, surgery is not recommended in women who want to conceive again because pregnancy and childbirth will disrupt any repair that has been performed. A pessary may be a better choice for these patients

Summary
Utero-vaginal Prolapse is a condition whereby the uterus protrudes down the vagina and sometimes out of the vaginal opening (introitus). There are 3 degrees of utero-vaginal prolapse. It may be associated with a cystocoele (descent of the bladder, a rectocoele (descent of the rectum) and/or enterocoele (descent of part of the intestines through the back part of the uterus). Treatment will depend on the symptoms ranging from just pelvic floor exercises, to using a pessary or surgery. Surgery can be done vaginally
or abdominally, with the aid of a laparoscope.
