Treatment for uterovaginal prolapse laparoscopically is a relatively new treatment modality. It has the benefits of an abdominal approach to the management of uterovaginal prolapse as well as a minimally invasive surgical technique. Laparoscopic surgery for uterovaginal prolapse can be performed with either a mesh or non-absorbable sutures. It may be done with or without the removal of the uterus.
1) Sacrocolpopexy
This is a surgery whereby a mesh is used to attach the vaginal vault, cervix or uterus to the sacral promontory (g). A mesh is a synthetic permanent material with many holes in it. It provides additional support by allowing the body’s own tissue to grow into it. When pelvic support structures are weak, the weakened tissues can be reinforced with a mesh. There are several ways of performing this surgery.

a) Subtotal hysterectomy and sacrocolpopexy.
This is believed to be the ideal surgery for uterovaginal prolapse. The technique involves the removal of the body of the uterus but the cervix is retained. The cervix is then attached to a mesh and the other end of the mesh is attached to the sacral promontory.

Laparoscopic subtotal hysterectomy and sacrocolpopexy for uterovaginal prolapse
http://vimeo.com/150044077
The technique
The peritoneum (g) overlying the sacral promontory is opened and the anterior longitudinal ligament is exposed. Care must be taken of the important structures that lay in this position, namely the right common iliac vessels, the medial sacral vessels and the right ureter. The peritoneum is then opened downwards on the right side of the sigmoid and extended up to the posterior part of the uterus. It is then extended to the left side over the rectum. The rectum is released from the vagina. A subtotal hysterectomy is then performed in the usual manner (see Chapter 33). A mesh is then attached to the cervix posteriorly. A second mesh is attached to the anterior part of the cervix or the upper part of the vagina if there is a cystocoele. The two meshes are then sutured together on either side taking the uterosacral ligaments with the suture. Excess anterior mesh is excised. The posterior mesh is then loosely sutured to the anterior longitudinal ligament of the sacral promontory. The peritoneum overlying the mesh is also then sutured together using absorbable sutures so as to completely cover the mesh.
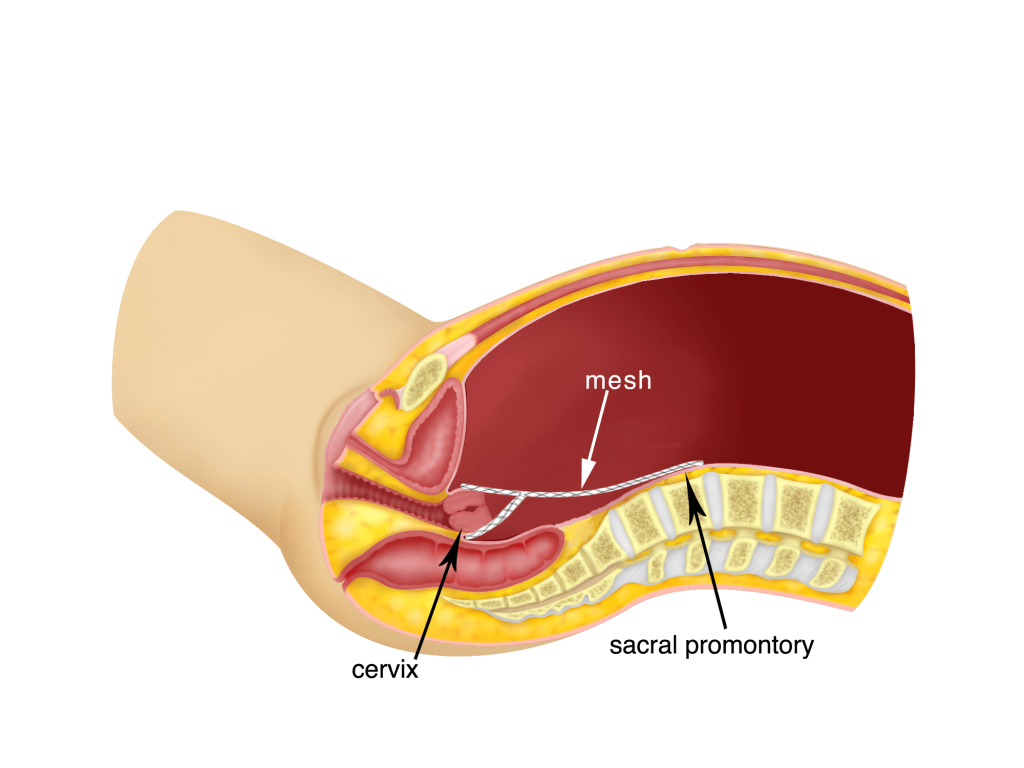
The advantages of this surgery are:
1) The cervix is a stronger structure to attach the mesh to as opposed to the vaginal vault, if a total laparoscopic hysterectomy was performed. There will be lesser incidence of mesh erosion into the vagina.
2) The chances of mesh infection would be lower as the vagina is not opened.
3) It is easier to suture two meshes (one in front of the cervix and one behind the cervix) when the body of the uterus is removed than when the uterus is retained.
Disadvantage
It is important for the patient to undergo regular pap smears to ensure that cervical lesions such as cervical dysplasia and cervical cancer do not occur, since the cervix is retained.
Complications
1) Mesh infection: Even when aseptic (g) techniques are used, there is always a possibility of mesh infection. This can be very troublesome. It may resolve with antibiotics but in severe cases, another surgery may be necessary for the removal of the mesh.
2) Infection of the sacral promontory and the cervical disc can also occur. This may resolve with antibiotics. Again in severe cases the mesh may have to be removed.
3) Mesh erosion into the vagina or rectum. The mesh may occasionally erode into the vagina causing pain during sexual intercourse. The patient may also suffer from spotting of blood vaginally because of the mesh erosion into the vagina. The protruding mesh can be excised vaginally and the vagina repaired or healed with oestrogen cream.
4) Recurrence of prolapse. In a small percentage of patients the surgery might fail and prolapse of the bladder (cystocoele), prolapse of the rectum (rectocoele) or even the cervix may occur.
b) Total Laparoscopic Hysterectomy and Sacrocolpopexy
In this technique, all the procedures performed are as in the Subtotal Hysterectomy and Sacrocolpopexy except that the uterus and cervix are removed. The vagina is opened to remove the uterus vaginally and the vaginal vault is closed. After that, a Y shaped mesh is used to suture the front and back part of the vault and then attached to the sacral promontory.
This technique can be performed when there is a worry of diseases of the cervix such as cervical dysplasia or cervical cancer. The disadvantage of this technique is that the chance of mesh infection is higher because the vagina has been opened. The risk of mesh erosion into the vagina is also higher.
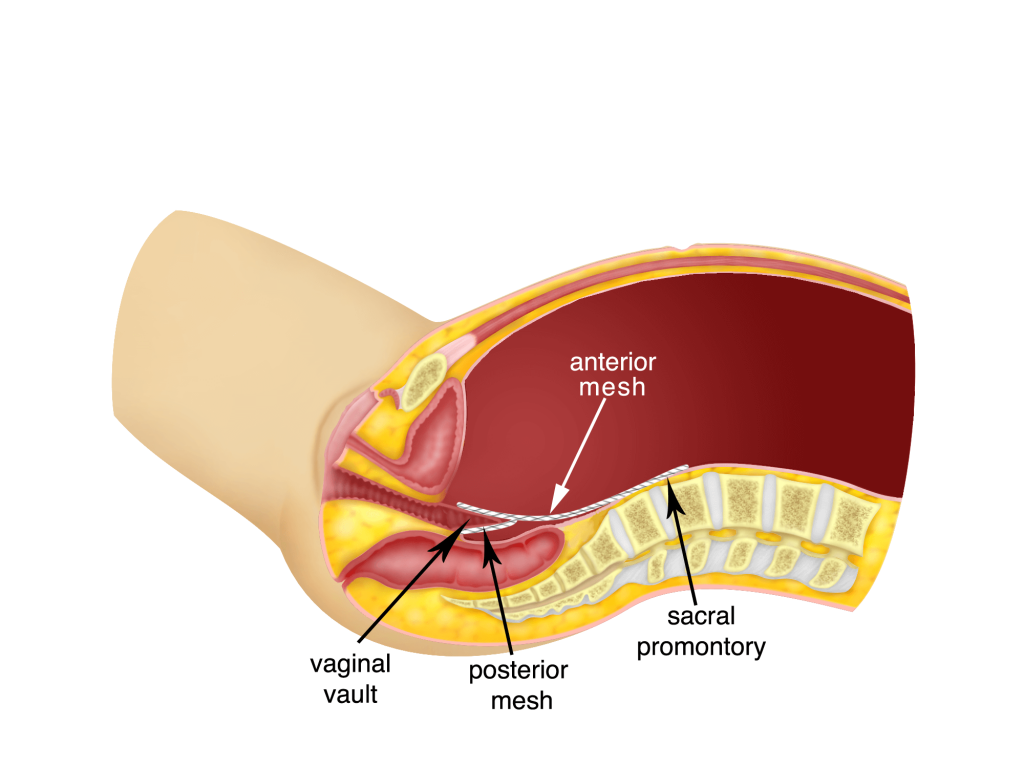
c) Sacrocolpopexy without Hysterectomy
In patients who wish to retain their uterus, Sacrocolpopexy can be performed. This technique is slightly more complex because of the difficulty in placing two meshes, one at the front or anterior surface of the uterus and the second behind or posterior to the uterus. The posterior mesh is then attached to the sacral promontory. This surgery can be performed on women who do not have any diseases of the uterus eg fibroids, adenomyosis, endometrial hyperplasia, cervical dysplasia and heavy menses (menorrhagia).
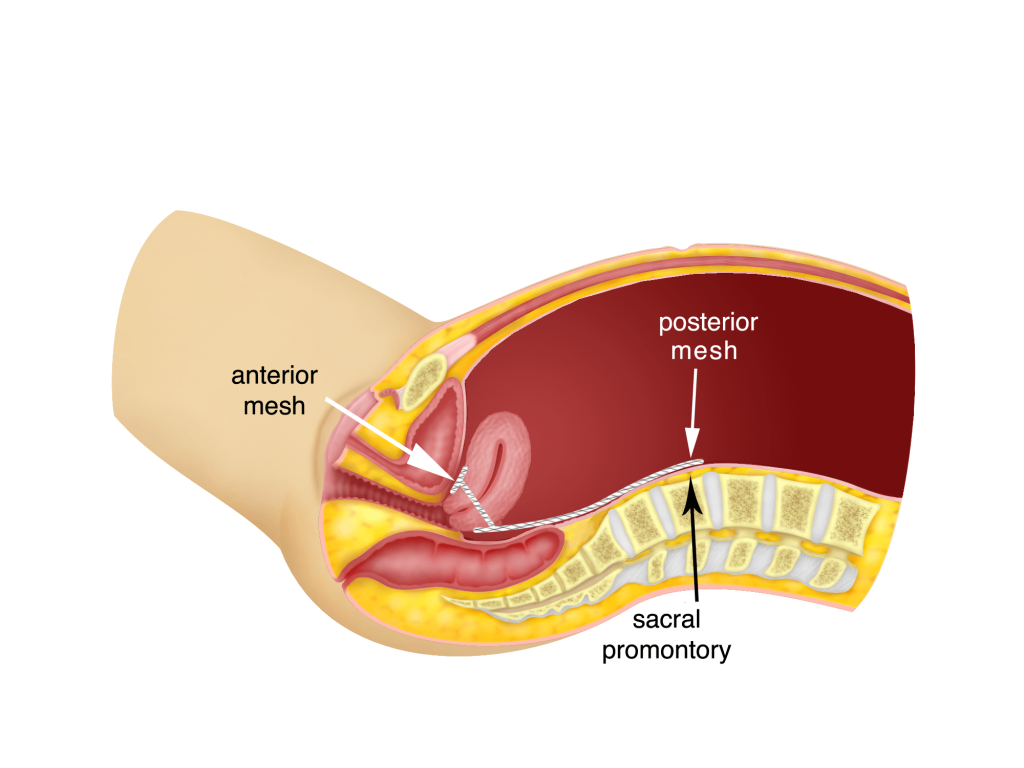
d) Post Hysterectomy Vaginal Vault Prolapse and Sacrocolpopexy
In patients who have vaginal vault prolapse (prolapse of the vaginal vault after a previous abdominal, vaginal or laparoscopic hysterectomy), Sacrocolpopexy can be performed. The technique is similar to the technique of Total Laparoscopic Hysterectomy and Sacrocolpopexy. The bladder and rectum is dissected away from the vaginal vault. Two meshes are used. The first is to suture the back (posterior) part of the vault to the muscles around the rectum (puborectalis muscle). The second mesh is sutured to the front (anterior) part of the vault. The two meshes are then sutured together to the vault. The other end is then sutured to the sacral promontory.
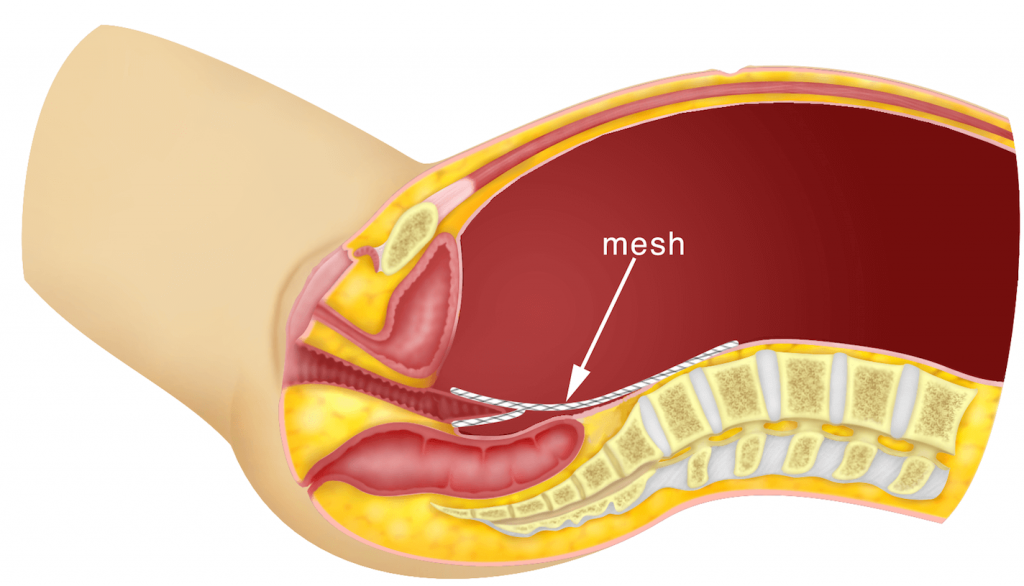

Case: 32.1 : Laparoscopic sacrocolpoplexy for vaginal vault prolapse
HAH was a 48 year old lady with three children who underwent a total abdominal hysterectomy at another hospital eight prior to consulting me in November 2014 . She came with severe vaginal vault prolapse. She did not have any stress incontinence. Examination and ultrasound showed that her ovaries were normal. After discussing various options for surgery she chose to undergo a laparoscopic sacrocolpoplexy. She underwent the surgery in December 2014. Postoperatively she has been well. (see Video 32.2)
Discussion
There are several ways of treating a vaginal vault prolapse. Laparoscopic Sacrocolpopexy is a good method especially in healthy young patients. It is a technically demanding surgery and requires advanced laparoscopic skills
2) Using non absorbable sutures
Dr. C Y Liu popularized this technique. This technique can be performed with or without the removal of the uterus. The principle of this technique is that, instead of using a mesh, non- absorbable sutures are used to support the uterus or vaginal vault. With a hand in the vagina against the right sacrospinous ligament, the sacrospinous ligament is identified laparoscopically. The peritoneum on the ligament is opened and the ligament
is exposed. A suture is placed into the right sacrospinous ligament and the suture is attached to the vaginal vault. This is repeated on the left side. Another suture is placed through the uterosacral ligaments and attached to the vaginal vault.
Summary
Laparoscopic surgery for uterovaginal prolapse is a relatively new procedure. It may involve the use of meshes to suture the cervical stump or vaginal vault to the anterior ligament of the sacral promontory or the use of sutures to suture the sacrospinous ligament to the vaginal vault. Postoperative recurrence of prolapse is believed to be lesser than the traditional vaginal hysterectomy and pelvic floor repair.
