There are many commonly used terms to describe the many different types of uterine abnormalities:
1) Hypoplasia/Agenesis
2) Unicornuate Uterus
3) Uterine Didelphus
4) Bicornuate Uterus
5) Septate Uterus
6) Arcuate Uterus
7) Diethylstilbestrol drug related
Development of the female reproductive tract
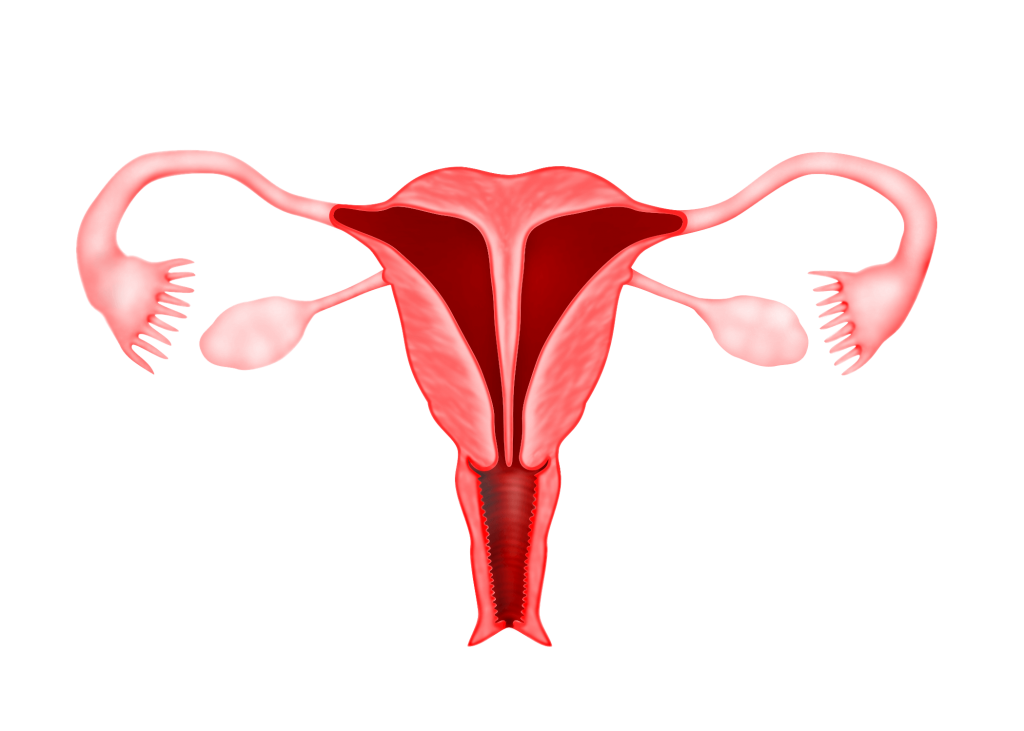
Sexual differentiation begins early in the foetal period of pregnancy (while a foetus is still in her mother’s womb). The male and female genital systems are identical up until the sixth week of life. There are two pairs of symmetrical genital ducts, the mesonephric (Wolffian) duct and the paramesonephric (Mullerian) ducts. The Wolffian ducts form the male reproductive system and the Mullerian ducts form the female reproductive system. In the female embryo, the Wolffian ducts begin to degenerate but allow the maturation of the Mullerian ducts. The two Mullerian ducts grow and fuse in the centre to become the uterus, ligaments and fallopian tubes. Congenital uterine abnormalities at this point occur because of a failure to complete the bilateral duct elongation, fusion, canalisation or septal resorption of the Mullerian ducts
1) Hypoplasia/Agenesis
Occurs when the uterus is not present. The vagina may or may not be present. This condition is known as Rokitansky-Kuster-Hauser syndrome.
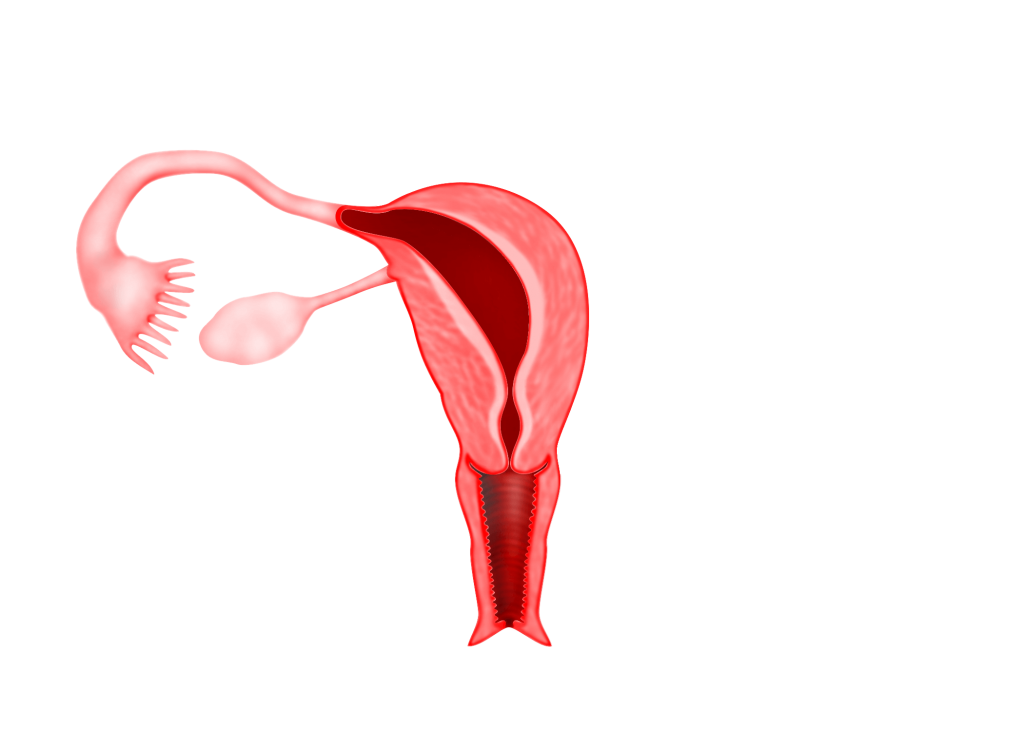
2) Unicornuate Uterus
Can be seen when only one side of the Mullerian duct forms. The uterus has a typical “penis shape” on imaging systems such as ultrasound or MRI. Sometimes it looks like
a rudimentary (simple) horn. If this rudimentary horn has a cavity, the patient may have unilateral cyclical pelvic pain, secondary to blood collecting in the cavity and being unable to flow out of the uterus. This condition has a high rate of spontaneous abortions and premature deliveries.
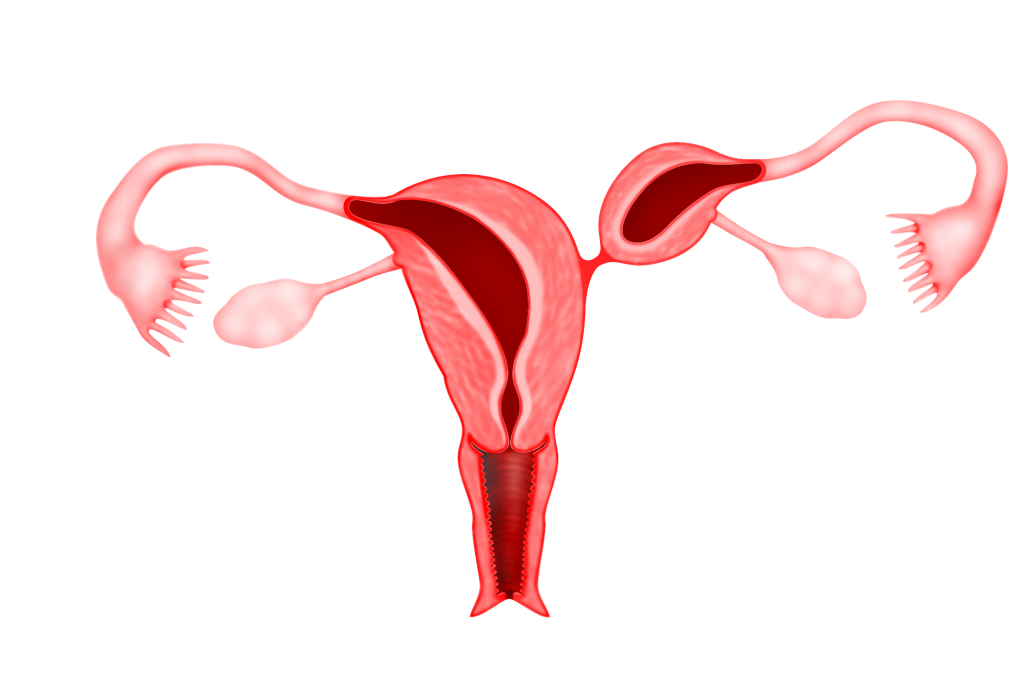
3) Uterine Didephus
Is evident when both the Mullerian ducts develop but fail to fuse, thus the patient has a “double uterus”. This may be a condition with a double cervix and a vaginal partition. Patients with this condition also have a higher incidence of spontaneous abortions and premature birth.
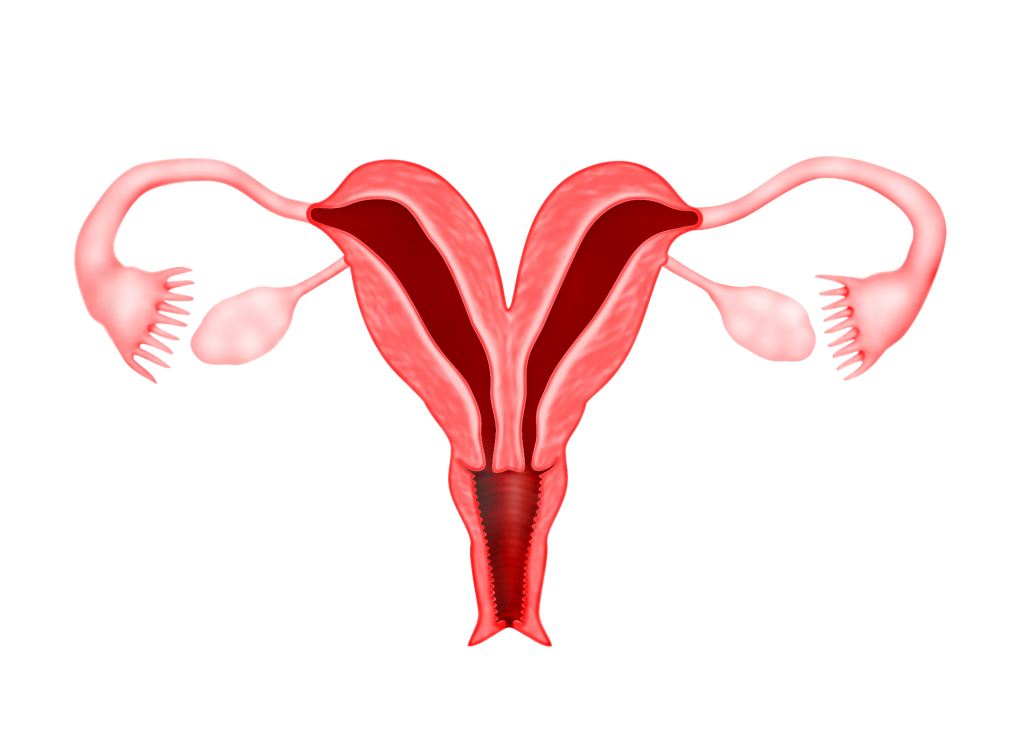
5) Septate Uterus
This happens when the two Mullerian ducts fuse, but the partition between them is still present, splitting the system into two parts. With a complete septum (g) the vagina, cervix and uterus can be partitioned. Usually the septum affects only the upper part of the uterus. A uterine septum is the most common uterine malformation and a cause for miscarriages. This condition can be corrected by hysteroscopy (see Chapter 40)
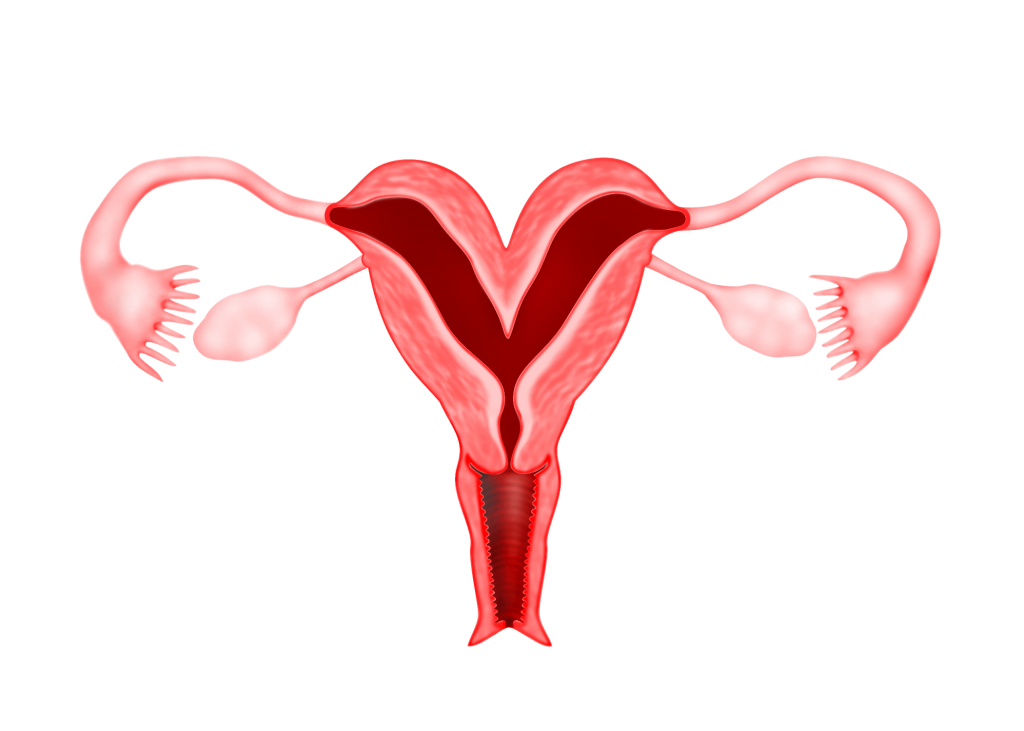
6) Arcuate Uterus
Occurs when the near-complete resorption of the uterovaginal septum leaves a mild concave indentation of the endometrial cavity, at the level of the fundus, giving the uterus an arcuate (g) configuration.
7) Diethylstilbestrol (DES) drug related
DES is an orally active synthetic oestrogen that was introduced in the 1940s for the treatment of recurrent pregnancy loss and premature delivery. Women exposed to this medication have children with uterine abnormalities and the most common abnormality is a T-shaped uterine cavity. Other abnormalities include a small uterus, constriction rings and intrauterine filling defects. This drug has been banned in the use in pregnancy since 1971.
Prevalence
The prevalence (incidence) of uterine malformation is estimated to be 6.7% in the general population. It is slightly higher (7.3%) in the infertility population, and significantly higher in the population of women with a history of recurrent miscarriages (16%).
Cause
In a majority of cases, the cause of a congenital uterine anomaly is unknown.
Symptoms
Many women with congenital uterine abnormalities have no symptoms. It is detected during a routine ultrasound examination. However, some symptoms women with uterine abnormalities may experience are:
1) Dysmenorrhoea – Pain during menses
2) Recurrent miscarriages or recurrent preterm deliveries
3) Primary amenorhoea – no menses at all
1) Dysmenorrhoea
Some women with uterine abnormalities may experience with severe pain during menses. There are several causes for this dysmenorrhoea. These women have a tendency to develop endometriosis, with blood in the fallopian tubes (hematosalpinx) and endometriotic cysts. In some women with a rudimentary horn and cavity, there is bleeding in the rudimentary cavity but there is no outlet for the menstrual blood to flow out of the vagina. This may cause pelvic pain during menses.
2) Recurrent miscarriages or recurrent preterm deliveries
Congenital uterine abnormalities are also more often seen in patients with recurrent miscarriages. The septate uterus is the most common abnormality and one with the worst reproductive outcome. However, this abnormality is the one most amenable to hysteroscopic correction.
3) Primary amenorhoea
There are several conditions that can cause a girl to not have her menses at all. Imperforate hymen is a simple condition in which there is no opening in a thickened hymen and menstrual blood collects in the vagina. This is easily diagnosed with an ultrasound scan and the hymen can be cut with 2 incisions like a cross (cruciate incision) to correct this condition. Other conditions are partial or complete absence of the vagina and absence of the cervix. These are more complex problems.
Case 11.1 : Twin pregnancies with IVF in a lady with a complete uterine septum
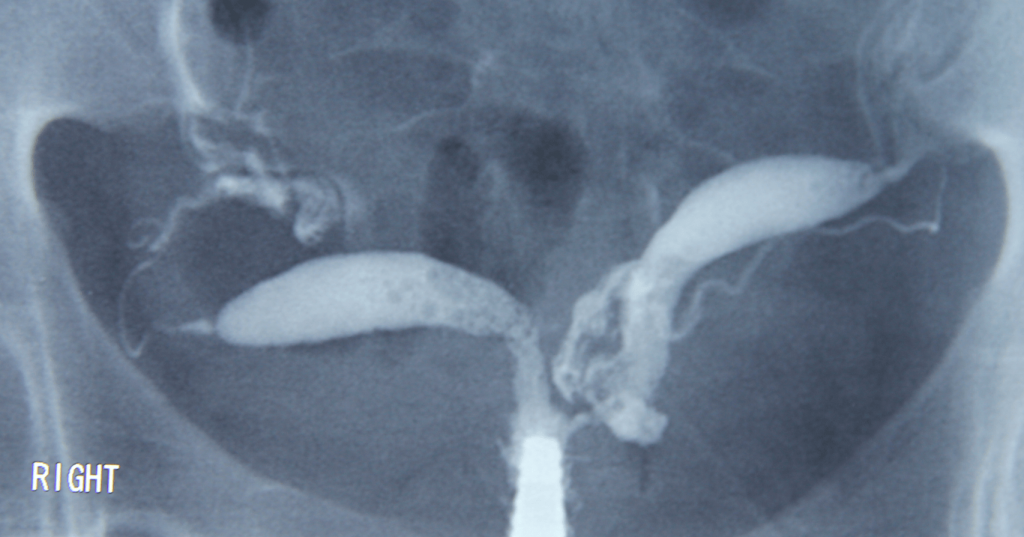
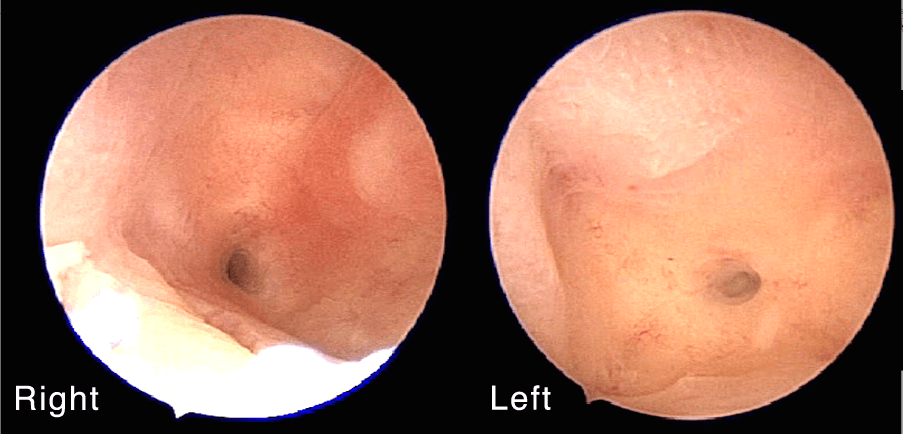
GWN, a 26 year old lady, saw me in 2001 for infertility. She had been married for 2 years. Examination and ultrasound showed a midline septum in the vagina. She also had double cervix. She underwent a laparoscopy and hysteroscopy. She had a single transversely elongated uterus with a complete vaginal midline septum and double cervix. She also had a complete midline uterine septum (Figure 11.4). Both the uterine cavities could be seen and were of normal size and capacity. Both fallopian tubes were patent (g). Incision of the vaginal septum was done. After the surgery she had difficulty conceiving. She received several courses of clomiphene citrate to induce ovulation but it was without any success. She underwent 2 cycles of intrauterine insemination (IUI) (g) without any success as well. In 2003 she underwent an invitrofertilization (IVF) cycle. One embryo was transferred into each uterine cavity and she conceived twins. She underwent an elective Caesarean section and delivered a pair of twins, a baby boy and a baby girl in 2004.
Discussion
Since this patient had double cervix, a midline complete uterine septum and 2 uterine cavities of normal size and capacity, a decision was made not to cut the uterine septum. If she had had only one cervix and a midline uterine septum, then excision of the uterine septum would have been an option to reduce the incidence of miscarriage.
Case 11.2 : Excision of non-communicating rudimentary horn of the uterus
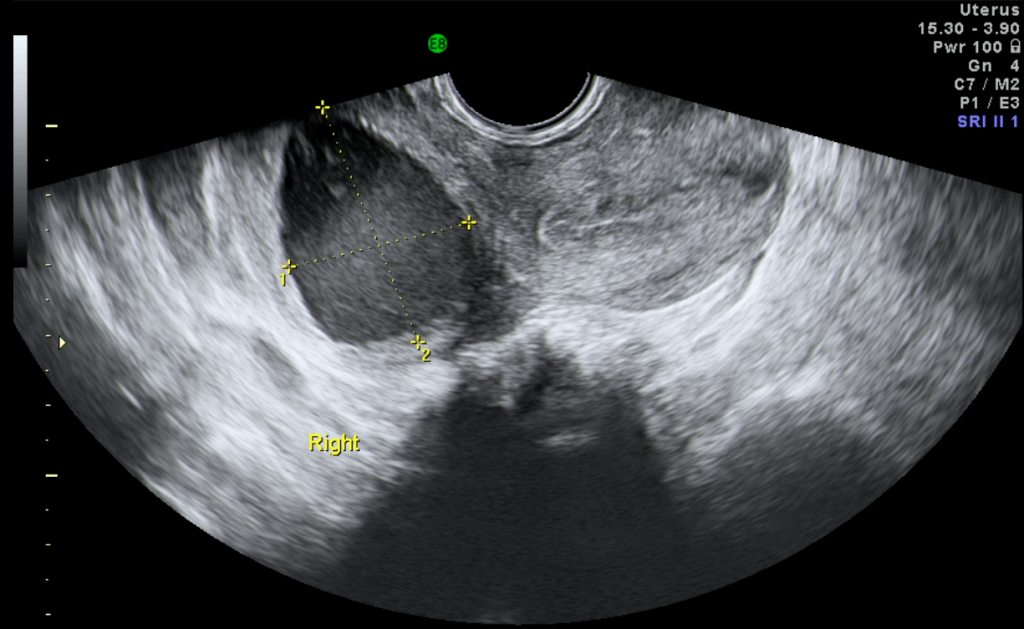
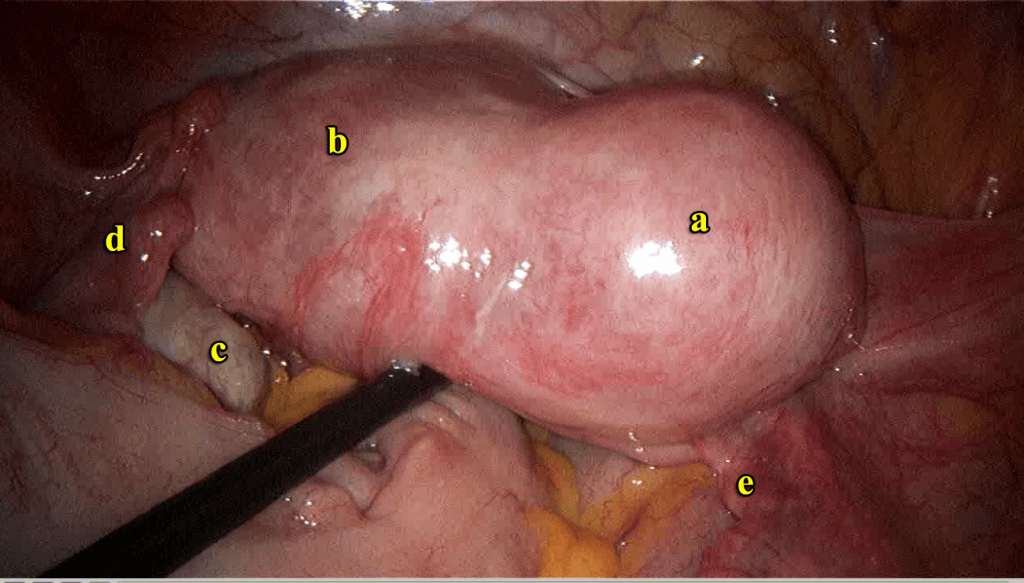
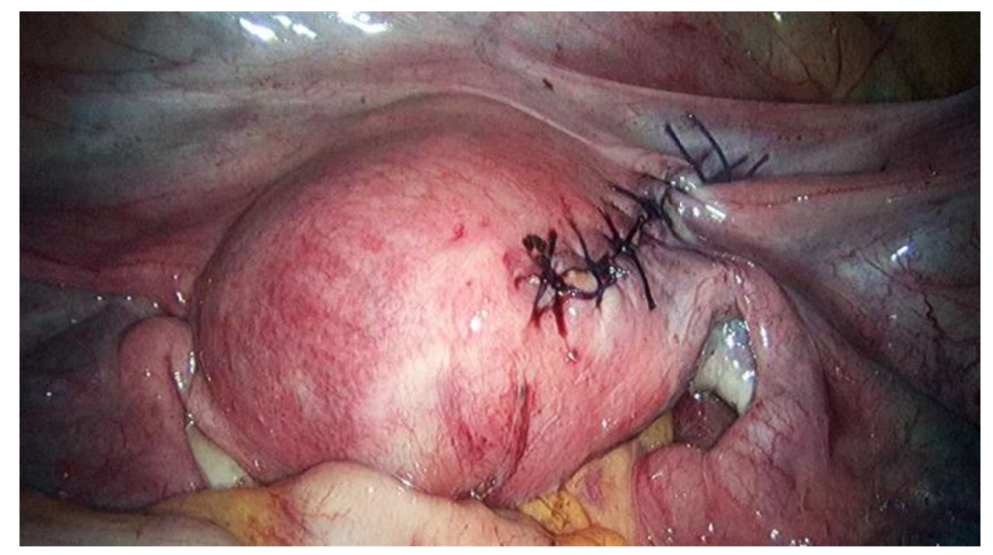
KV, a 22 year old lady who had not had sexual intercourse before (virgo intacta), presented with a history of pain after menses for 3 months. She attained menarche at the age of 15 and never had dysmenorrhea before. Her menstrual flow was normal and regular. Transabdominal ultrasound showed a cystic mass measuring 2.80 x 3.16 cm on the right side, which appeared like a right endometrioma (Figure 11.11). She underwent a laparoscopy. A globular swelling was found attached to the uterus on the right side (Figure 11.12). The ovaries and fallopian tubes were normal. The right fallopian tube appeared to arise from the uterus and not from the globular mass. There was minimal endometriosis on the back (posterior) aspect of the uterus. A needle was used to aspirate the mass and brownish fluid resembling endometriosis was obtained. She was diagnosed with non- communicating uterine horn. As I did not have any consent to excise the uterine horn I did not proceed with the excision of the rudimentary horn. The findings were discussed with the patient and her parents. She underwent a magnetic resonance imaging (MRI) scan, which clearly showed that the mass was a non-communicating rudimentary horn. I obtained consent to perform a hysteroscopy during the second laparoscopy. The hysteroscopy was performed without injuring the hymen and a dye was injected directly into the right tubal ostium. The right tube was found to be patent. The uterine horn was then excised and the defect sutured (Figures 11.2 and 11.3). Postoperatively, she has been well with no dysmenorrhea. (watch video 11.2 Excision of non-communicating rudimentary horn)
Discussion
There are many reasons for having pain during menses (dysmenorrhea). In this patient a cystic mass was seen on transabdominal ultrasound. As the right ovary could not be visualised, it was assumed that the lesion was an endometrioma. A transvaginal ultrasound would have clearly shown the right ovary and that this lesion was part of the uterus and not the ovary. When a cystic mass is seen on ultrasound, one must not conclude that it is of ovarian origin. In a virgo inacta patient where a transvaginal ultrasound cannot be done and a transabdominal ultrasound can be misleading, a 3 D ultrasound or MRI can confirm the diagnosis of a non communicating rudimentary horn.
Diagnosis
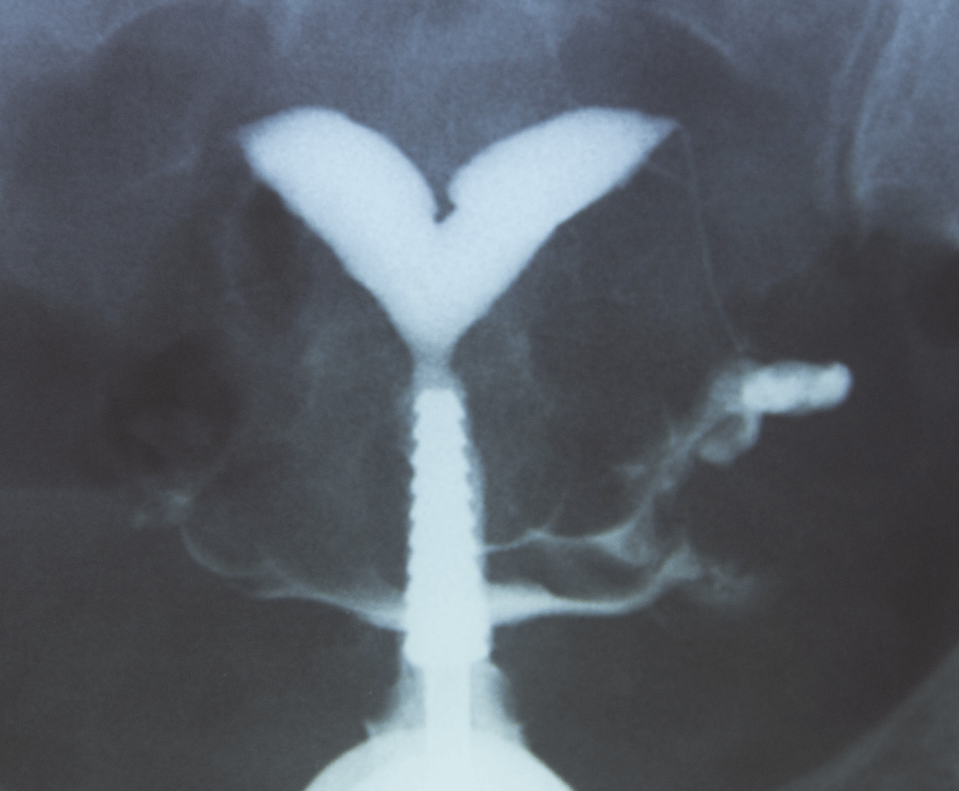
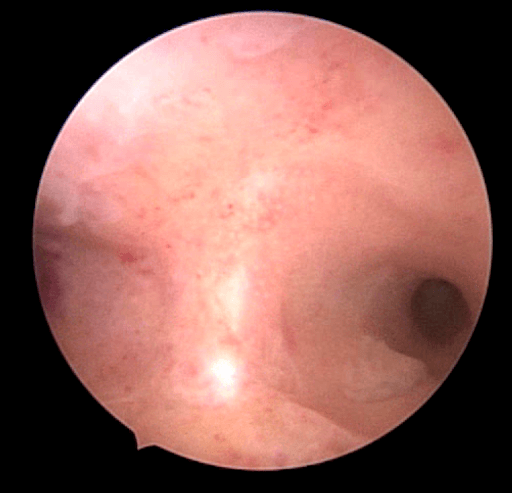
Diagnosis of uterine abnormalities can be done with a routine ultrasound. Uterine didelpus and bicornuate uterus can be easily seen on a 2D ultrasound. A septate uterus can be more difficult to diagnose with a 2D ultrasound but can be confirmed with a MRI or a 3D ultrasound (especially if addition of fluid in the cavity is done while performing the 3D ultrasound). Sometimes a diagnosis of uterine abnormalities can be made on a routine hysterosalpingogram (HSG). A diagnostic hysteroscopy can also confirm the diagnosis of uterine abnormalities (see Chapter 40). It is important to note that women with uterine abnormalities may also have abnormalities of the renal system such as the absence of one kidney or have abnormal kidneys or abnormally placed kidneys.
Treatment
Treatment will depend on the symptoms of the patient. Many patients with uterine abnormalities will not require any treatment at all. They will be able to conceive spontaneously and will be able to carry the foetuses to full term and deliver the baby normally. However, surgery may be indicated in the following conditions:
1) Dysmenorrhoea
In patients with a rudimentary cavity, laparoscopic surgery can be performed to remove the rudimentary horn. In patients with a rudimentary horn which is in communication with the fallopian tubes but not the vagina, endometrioma and hematosalpinx, may occur. In these patients removal of the uterine horn will cure the disease.

2) Recurrent abortions or recurrent preterm deliveries
Uterine septum is the most common congenital uterine abnormality that causes recurrent abortions or recurrent preterm deliveries. Other causes are unicornuate uterus or bicornuate uterus. These conditions used to be corrected by a surgery called metroplasty, in which the septum is removed laparoscopically or by laparotomy and the uterine cavity is unified. This surgery is rarely performed now. Hysteroscopic resection of the septum is the operation of choice now (see Chapter 40 – Septoplasty)

Summary
Many women with congenital uterine abnormalities do not know that they have this condition. They do not have any medical or gynaecological problems and conceive and deliver their babies normally. These abnormalities may be diagnosed during a routine ultrasound. However in patients with recurrent miscarriages, preterm deliveries or infertility (if such conditions are diagnosed), surgical treatment may be contemplated. The best surgery available now is hysteroscopic resection of a uterine septum. This can be done with the assistance of an ultrasound or laparoscopy.
